Japanese Journal of Gastroenterology Research
Review Article - Open Access, Volume 2
The natural history of untreated coeliac disease, and why it matters
Jonathon Snook
Gastroenterology Unit, Poole Hospital - United Hospitals Dorset, UK.
*Corresponding Author : Jonathon Snook
Gastroenterology Unit, Poole Hospital - United
Hospitals Dorset, UK.
Email: jonathon.snook@gmail.com
Received : Sep 20, 2022
Accepted : Oct 10, 2022
Published : Oct 17, 2022
Archived : www.jjgastro.com
Copyright : © Snook J (2022).
Abstract
Coeliac Disease (CD) is a common, chronic inflammatory disorder of the small bowel triggered by exposure to dietary gluten. Much is known about the pathogenesis of CD, with strong evidence implicating immune reactivity to both gliadin-related peptides and autoantigens.
The natural history of CD is not well understood however-and so there remains uncertainty about whether it is an acquired condition, and if so, whether this acquisition is for life. This paper proposes the linked hypotheses that (1) CD is an acquired disorder, and (2) in those who do acquire it, there is a dynamic equilibrium between glutentolerant and gluten-reactive states. It goes on to outline and evaluate the available evidence addressing these important issues.
Strong circumstantial evidence favours the hypothesis that gluten immune reactivity is indeed acquired, requiring not only genetic predisposition and gluten exposure, but also the influence of one or more environmental factors on development of the CD phenotype. Similarly, there is strengthening evidence that immune reactivity to gluten can be lost, possibly leading to a dynamic equilibrium between immune reactive and immune tolerant states.
The conclusions that CD is acquired and isn’t necessarily life-long have major implications for the diagnosis and management of CD. The important caveat remains however that until the relationship between states of tolerance and reactivity are better understood, and we have reliable non-invasive methods of determining current gluten immune reactivity regardless of gluten intake, the safest option remains for established coeliacs to stay on a gluten-free diet indefinitely.
Keywords: Coeliac disease; Genetics; Autoimmunity; Gluten.
Abbreviations: CD: Coeliac Disease.
Citation: Snook J. The natural history of untreated coeliac disease, and why it matters. Japanese J Gastroenterol Res. 2022; 2(13): 1113.
Introduction
Coeliac Disease (CD) is a common, chronic inflammatory disorder of the small bowel triggered by exposure to dietary gluten, in the context of an immunological reaction against both exogenous and auto-antigens. It has a series of important consequences including malabsorption leading to diarrhoea and weight loss, nutrient deficiencies resulting in anaemia and accelerated osteoporosis, and (on occasion) small bowel malignancy [1-3].
Much is known about the pathogenesis of CD. Overwhelming evidence implicates the immune response in this process, including the strong link with HLA alleles DQ2 and DQ8, the association with other autoimmune disorders, anintense mucosal lymphocytic infiltrate on histological examination of the small bowel mucosa, and the frequent finding of circulating anti-gliadin and anti-endomysial antibodies in untreated CD [1-3].
The natural history of the condition is however far less well understood, and there are several reasons for this. Firstly, the correlation between symptoms and disease activity is poor, meaning that the former are not a reliable marker of the latter. Secondly, the small bowel mucosa is relatively inaccessible, and so it generally isn’t feasible to take serial biopsies for histology - the gold standard test for CD [1-3]. Finally, standard medical advice following the diagnosis of CD is to adopt a long-term gluten free diet to minimise the risk of disease complications-with the express intention of modifying the disease course.
As a consequence there remains uncertainty about two key issues concerning the natural history of the condition. The first is whether CD is an acquired disorder, and the second is if acquired, whether it is for life. This paper evaluates the available evidence addressing these important questions. For the purposes of the article, CD is defined as a tendency to gluten reactivity, so that a previously diagnosed individual with normal mucosa on a gluten free diet would still be considered to have the condition.
Discussion
Is coeliac disease an acquired condition?
It was established back in the last century that the trigger for the immune activation which characterises CD is mucosal exposure to dietary gluten in genetically predisposed individuals. Since gluten exposure is almost universal after weaning in wheat-consuming populations, this simple two-factor model of disease - gluten plus genes -implies that CD is in effect constitutional. It fits with the classical picture of a young, malnourished child with the disorder as originally described by Samuel Gee [4], and with evidence confirming the clinical impression that those diagnosed with CD in later life sometimes have a history of indicative symptoms and / or laboratory abnormalities for many years prior[5].
There are however multiple lines of evidence which do not fit with this model. Most fundamental, many people at high genetic risk do not develop CD despite gluten exposure. Estimates from sero-prevalence studies are that in most gluten-exposed populations 1-2% have CD, whether formally diagnosed or not - whilst up to40% of individuals in these populations carry one or more of the high-risk HLA DQ genes [1-3].
So how is this disparity explained? The influence of other genes needs to be considered, and there is evidence for a non-HLA related genetic contribution to risk from genome-wide association studies [6]. Even genetic studies have concluded however that environmental factors in addition to gluten exposure make a significant contribution to the risk of CD [1-3,6], and a series of other lines of evidence support that conclusion.
Firstly, early descriptions of monozygotic twin pairs discordant for CD on the basis of histology [7,8] have subsequently been confirmed by formal twin studies [9,10], with serological and/or histological exclusion of concordance in 29-51% of monozygotic pairs. Consistent with this are case-series describing individuals at high genetic risk who had normal small bowel histology on initial assessment, only to develop biopsy-proven CD at a later date [11,12].
Secondly, rather more cases of CD are diagnosed in adults than children. A recent study of 802 incident cases in a defined population including children revealed a median age at diagnosis of 50, with 36% being over the age of 60 [13]. Delayed diagnosis of CD is of course a well-recognised phenomenon [5] and so the submerged element of the “coeliac iceberg” representing atypical and silent forms of CD [14] may have contributed to this observation. If this was a major factor however, the expectation would be a substantial fallin the age at diagnosis with the development of widespread (and increasingly untargeted) serological screening for CD in many populations over the last three decades [1-3]. In fact, there has been little change [13].
Thirdly, whilst anaemia is a common manifestation of untreated CD [13], the interval between onset of anaemia and diagnosis of CD appears to be relatively short. A data linkage study of 1.1 million Swedish blood donors identified 1567 individuals diagnosed with incident CD during the follow-up period. Compared with matched controls, the average duration of anaemia pre-diagnosis was just 1.4 years (95% CI: 1.1-2.1 years) [15].
Fourthly, a series of independent studies and a subsequent meta-analysis [16,17] have identified an association with cigarette smoking, showing an apparent protective effect of smoking compared to never-smoking, with some evidence of a dose-effect relationship [16]. Association does not of course prove causation, and as there will obviously never be a randomised controlled trial, a range of explanations for this observation need to be considered. It is conceivable that undiagnosed CD could in some undefined way dissuade individuals from taking up smoking, or that some unidentified confounder predisposes to both CD and non-smoking. Alternatively, smoking might somehow reduce the probability of an individual being diagnosed with CD, though the under-representation of smokers in seropositive populations with undiagnosed CD makes this explanation unlikely [18].
The remaining interpretation is that smoking modulates the risk of developing CD. This has some plausibility, given the well-established influence of cigarette smoking on other inflammatory enteropathies, Crohn’s disease and ulcerative colitis [19] (albeit with a different relationship pattern), and a range of other autoimmune disorders [20]. The mechanism is unknown, but effects on intestinal permeability, the immune system and / or the micro biome may be operative.
Finally, clustering of cases of CD in space and time has been reported. A population study in Sweden reported a fourfold increase in the incidence of CD in children under 2 between 1985 and 1987, with a subsequent sharp reversion to previous rates after 1995 [21]. A subsequent study identified two waves in the incidence of CD across all age-groups in the same country, with peaks in the early 1990s and early 2000s, and subsequent falls [22]. Meanwhile, case clustering was reported in a town in the south of England in a time window between 1998 and 2002, with an incidence almost three-fold greater than expected [23]. This temporo-spatial case clustering clearly cannot be accounted for by changes in the gene pool or gluten exposure, and although variable case ascertainment is a potential confounder in observational studies of this type, it is difficult to accept this as the explanation for such marked variation.
This series of observations collectively point strongly to the presence of a third pre-requisite for the development of CD, in addition to genes and gluten. This third element is likely to be an environmental factor, accounting for the observations on age at diagnosis and temporo-spatial clustering, and the apparent link with smoking. Enteric viral infections are an attractive explanation, and evidence has been published implicating a range of potential candidates including rotavirus [24], reovirus [25]and enterovirus [26] without conclusive proof. Considering the question of a viral trigger it will be interesting to assess the influence of lockdowns resulting from the SARS-CoV-2 pandemic since 2020 on the subsequent incidence of CD, given the profound effect on gastro-intestinal infection rates [27].
In summary, the evidence strongly favours the hypothesis that coeliac disease is an acquired disorder requiring not only predisposing genes and gluten exposure, but also a third factor with an environmental basis, as yet unidentified.
Is coeliac disease really for life?
Many authorities refer to CD as a state of permanent gluten intolerance, and standard practice is to recommend a life-long gluten free diet once an individual is diagnosed. The aim of this is to establish and maintain histological remission, and to minimise the risk of long-term complications [1-3].
But is the blanket dogma “once a coeliac, always a coeliac” evidence-based? Whilst in some cases CD undoubtedly reactivates on re-exposure to gluten, is this invariably the case? If not, does this mean that some people remain on a gluten-free diet unnecessarily? And if so, can we identify these individuals? These questions have been raised before [28], but recent additions to the literature have strengthened the evidence base, as outlined below.
A major difficulty in trying to answer these questions is that we generally don’t get an opportunity to follow the natural history of CD after diagnosis, primarily because most people adopt a life-long gluten-free diet following standard advice from their physician. There are however two situations where individuals with confirmed CD are re-exposed to gluten – the first by electing not to comply with dietary restriction in the longer term, and the second by volunteering to undergo gluten challenge in an experimental setting.
Whilst non-compliant coeliacs tend to be a challenging group to follow up [29], there are now three published case-series describing the findings on re-investigation of individuals with a confident diagnosis of CD earlier in life, who have subsequently opted to revert to a gluten-containing diet [30-32]. Interestingly, the prevalence of normal small bowel histology in these series ranged from 21% to 67% (Table 1). Most cases reported were originally diagnosed in childhood, and it remains to be established whether the same applies to CD diagnosed in adulthood.
Table 1: The prevalence of normal small bowel histology in previously diagnosed coeliacs who elected to revert to a gluten-containing diet.
Reference |
Age (years) at : |
Duration of |
Normal histology |
|
Diagnosis |
Re-investigation |
|||
Matysiak-Budnik et al |
0 - 16 |
17 - 53 |
2 - 44 |
13/61 (21%) |
Hopman et al |
0 - 32 |
22 - 66 |
1 - 34 |
8/12 (67%) |
Norsa et al |
0 - 25 |
31 - 65 |
Not specified |
20/34 (59%) |
A series of gluten challenge studies have been reported over the years, looking at a variety of parameters to assess immune reactivity in individuals with a confident diagnosis of CD in established remission on a gluten-free diet [33-41]. Regardless of the magnitude or duration of the gluten challenge, and the number and nature of the parameters assessed, 7-27% of cases proved to be gluten non-reactive (Table 2).
Table 2: Summary of gluten challenge studies in established coeliacs.
Reference |
Gluten challenge g/day (days) |
Parameters assessed |
Non-responders by |
Maki et al |
Not specified |
Histology and serology |
4/29 (14%) |
Burgin-Wolff et al |
Not specified |
Histology |
24/134 (18%) |
Anderson et al (2005)[35] |
8 (3) |
Immunoreactive PBTLs |
9/59 (15%) |
Lähdeahoet al(2011) [36] |
1 – 5 (84) |
Histology and serology |
4/21 (19%) |
Leffler et al(2013) [37] |
3.0 / 7.6 (28) |
Histology and serology |
2/19 (11%) |
Sarna et al |
5.7 (14) |
Histology, serology, HLA-tetramer and cytokines |
3/15 (20%) |
Goel et al |
10 (1) |
Serum IL-2 |
3/25 (12%) |
Schuppan et al |
3 (42) |
Histology – villous-crypt ratio |
8/30 (27%) |
Leonard et al(2021) [41] |
3 or 10 (14) |
Histology, serology, HLA-tetramer and IL-2 |
1/14 (7%) |
The findings of both sets of studies do of course raise some challenging questions about the accuracy of the original diagnosis of CD, and the rigour with which “normality” on follow-up testing was defined. Furthermore, self-selection might bias the findings of the case series of non-complaint coeliacs, as those who either lost or never truly had a predisposition to gluten immune reactivity are perhaps more likely to tolerate a gluten-containing diet. Nevertheless, the collective data from observational studies of non-compliant coeliacs and experimental gluten challenge in compliant ones would suggest that a significant minority have spontaneously restored gluten tolerance, and therefore that in some cases at least, CD is not a lifelong condition.
How does this conclusion marry with the observation that the seroprevalence of undiagnosed CD in population studies is remarkably constant across successive age-band cohorts? [18,42]. The reconciling explanation appears to have been provided by a study of healthy 15551 adults in Olmsted County, Minnesota, who each provided two blood samples taken a median of 8.8 years apart. These were analysed retrospectively [43]. Excluding those who adopted a gluten-free diet in the interim, 41 of 127 who were seropositive on the first sample became seronegative on the second, almost exactly matched by 49 original seronegatives who became seropositive-so that the overall seroprevalence in the cohort changed little over the duration of the study.
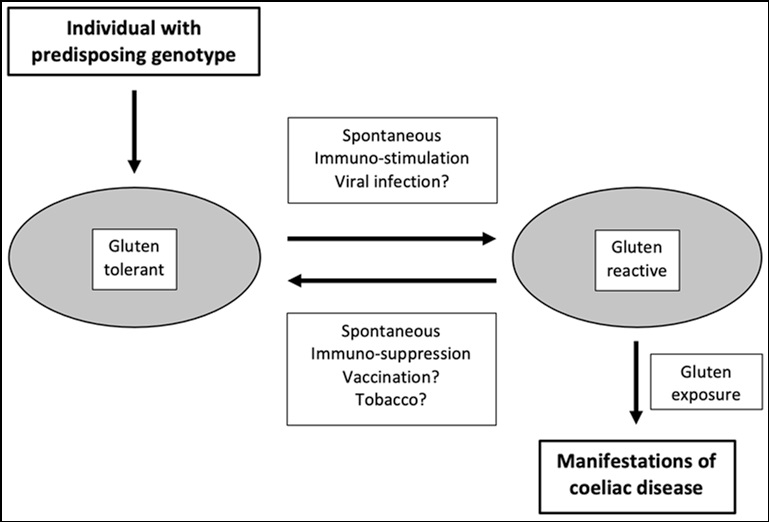
The implication from this collection of observations is that in those with a genetic predisposition to CD, there may be a dynamic equilibrium between gluten tolerant and gluten reactive states (Figure 1). This is perhaps not be surprising, given that CD meets the criteria for an autoimmune disorder, and that many other autoimmune conditions such as autoimmune thyroid disease, primary sclerosing cholangitis, systemic lupus erythematosus and inflammatory bowel disease typically follow a relapsing/remitting course, with periods of spontaneous and sometimes sustained remission. Whilst coeliac serology is not a perfect marker of histological activity in CD, this concept is also consistent with the striking fluctuations seen in coeliac antibody levels in children at high genetic risk of CD, with the spontaneous loss of seropositivity in up to 50% of cases despite ongoing gluten exposure [44-46].
There are two pre-requisites for accepting that CD is not always for life. The first is that the disorder not constitutional, as addressed in the previous section. The second is that it is fully reversible, and we know that this is the case from observations of coeliacs who continue to ingest gluten following treatment with immune suppression [47] and perhaps vaccination [48]. Evidence from the Minnesota study suggests that reversal of the disease process may also happen as a spontaneous event [43].
The nature of other factor(s) influencing the dynamic equilibrium between gluten reactive and gluten tolerant states in those with a genetic predisposition are not well understood. They may include tobacco exposure [16,17], inter current viral infections [24-26], and exposure to other medications including therapy with immune modulators such as interferon [49] and immune checkpoint inhibitors [50] (Figure 1). There is some evidence to suggest that the microbiome might also be involved [51].
Future research
Further work is clearly needed to confirm or indeed refute the hypotheses presented here, with a focus on defining the natural history of untreated CD. This raises a potential conflict with the conventional dogma of placing everyone diagnosed with CD on a lifelong gluten-free diet. Adherence to a gluten-free diet does however have significant practical, financial and psychological implications for the individual concerned, and it is well established that compliance in the longer term is therefore limited [52]. Furthermore, whilst the laudable aim of a universal gluten-free approach is to reduce the risk of complications, the objective evidence that it actually does so is poor.
Conclusion
In conclusion, the natural history of CD is less well understood than the pathogenesis of the condition. However, the evidence would suggest that like many autoimmune conditions, CD is not constitutional but in fact an acquired disorder with genetic predisposition. This has two important practical implications. Firstly, it means that a negative test for CD cannot rule out the diagnosis for life. Secondly, it makes intervention to reverse gluten reactivity by blocking the action of the triggering environmental factor a realistic aim.
The evidence would further suggest that in genetically predisposed individuals, there may be a dynamic equilibrium between gluten tolerance and gluten reactivity. Remission due to spontaneous loss of gluten reactivity may in fact be a relatively common event, meaning that at any given time, a proportion of previously diagnosed coeliacs may be following a gluten free diet despite no longer being gluten reactive.
Further investigation is clearly needed to characterise the balance between gluten tolerance and reactivity, and to define the factors that influence it. Until this process is understood, and we have reliable non-invasive methods of determining current gluten immune reactivity regardless of gluten exposure, the safest option of course remains for established coeliacs to remain on a gluten-free diet indefinitely.
References
- Hopper AD, Hadjivassiliou M, Butt S. Adult coeliac disease. BMJ. 2007; 335: 558-562.
- Di Sabatino A, Corazza GR. Coeliac disease. Lancet. 2009; 373 : 1480-1493.
- Lebwohl B, Sanders DS, Green PHR. Coeliac disease. Lancet. 2017; 391: 70-81.
- Dowd B, Walker-Smith J. Samuel Gee, Aretaeus, and The Coeliac Affection. Br Med J. 1974; 2: 45-47.
- Vavricka SR, Vadasz N, Stotzt M, Lehmann R, Studerus D, et al. Celiac disease diagnosis still significantly delayed - doctors’ but not patients’ delay responsible for the increased total delay in women. Dig Liver Dis. 2016; 48: 1148-1154.
- Van Heel DA, Franke L, Hunt KA, Gwilliam R, Zhernakova A, et al. A genome-wide association study for celiac disease identifies risk variants in the region harboring IL2 and IL21. Nat Genet. 2007; 39: 827-829.
- Walker-Smith JA. Discordance for childhood coeliac disease in monozygotic twins. Gut. 1973; 14: 374-375.
- Hoffman HN, Wollaeger EE, Greenberg E. Discordance for nontropical sprue (adult celiac disease) in a monozygotic twin pair. Gastroenterology. 1966; 51: 36-42.
- Nisticò L, Fagnani C, Coto I, Percopo S, Cotichini R, et al Concordance, disease progression, and heritability of coeliac disease in Italian twins. Gut. 2006; 55: 803-808.
- Kuja-Halkola R, Lebwohl B, Halfvarson J, Wijmenga C, Magnusson PKE, et al Heritability of non-HLA genetics in coeliac disease: a population-based study in 107 000 twins. Gut. 2016; 65: 1793- 1798.
- Maki M, Holm K, Koskimies S, Hallstrom O, Visakorpi JK. Normal small bowel biopsy followed by coeliac disease. Arch Dis Child.1990; 675: 1137-1141.
- Auricchio R, Mandile R, Del Vecchio MR, Scapaticci S, Galatola M, et al. Progression of Celiac Disease in Children With Antibodies Against Tissue Trans glutaminase and Normal Duodenal Architecture. Gastroenterology. 2019; 157: 413-420.
- Stroud C, Almilaji O, Nicholas D, Kirkham S, Surgenor SL, et al. Evolving patterns in the presentation of coeliac disease over the last 25 years. Frontline Gastroenterology. 2020; 11: 98-103.
- Catassi C, Ratsch IM, Fabiani E, Rossini M, Bordicchia F, et al. Coeliac disease in the year 2000: exploring the iceberg. Lancet. 1994; 343: 200-203.
- Ludvigsson JF, Sjölander A, Murray JA, Hjalgrim H, Edgren G, et al. Haemoglobin decline before coeliac disease diagnosis: a nationwide transfusion cohort study of 1.1 million blood donors. Gut. 2017; 66: 2036-2037.
- Suman S, Williams EJ, Thomas PW, Surgenor SL, Snook JA. Is the risk of adult coeliac disease causally related to cigarette exposure? Eur J Gastroenterol Hepatol. 2003; 15: 995-1000.
- Wijarnpreecha K, Lou S, Panjawatanan P et al. Cigarette smoking and risk of celiac disease: a systematic review and meta-analysis. United European Gastroenterol J. 2018; 6: 1285-1293.
- West J, Logan RF, Hill PG, Cheungpasitporn W, Pungpapong S, et al. Seroprevalence, correlates, and characteristics of undetected coeliac disease in England. Gut 2003; 52: 960-965.
- Parkes GC, Whelan K, Lindsay JO. Smoking in inflammatory bowel disease: Impact on disease course and insights into the aetiology of its effect. Journal of Crohn’s and Colitis. 2014; 81: 717 - 725
- Costenbader KH, Karlson EW. Cigarette smoking and autoimmune disease : what can we learn from epidemiology? Lupus 2006; 15: 737-745.
- Ivarsson A, Persson LA, Nystrom L. Epidemic of coeliacdisease in Swedish children. Acta Paediatr. 2000; 89: 165 - 71
- Bergman D, King J, Lebwohl B, Clements MS, Roelstraete B, et al. Two waves of coeliac disease incidence in Sweden: a nationwide population-based cohort study from 1990 to 2015. Gut. 2022.
- Fowell AJ, Thomas PW, Surgenor SL, Snook JA. The epidemiology of coeliac disease in East Dorset (1993-2002): an assessment of the coeliac iceberg, and preliminary evidence of case clustering. Quarterly J Medicine. 2006; 99: 453-460.
- Stene LC, Honeyman MC, Hoffenberg EJ, Haas JE, Sokol RJ, et al. Rotavirus infection frequency and risk of celiac disease autoimmunity in early childhood: a longitudinal study. Am J Gastroenterol. 2006; 101: 2333-2340
- Bouziat R, Hinterleitner R, Brown JJ, Tencel-Baerenwald JES, Ikizler M, et al. Reovirus infection triggers inflammatory responses to dietary antigens and development of celiac disease. Science 2017; 356: 44-50.
- Kahrs CR, Chuda K, Tapia G, Stene LC, Mårild K, et al. Enterovirus as trigger of coeliac disease: nested case-control study within prospective birth cohort. BMJ. 2019; 364: 272.
- Love NK, Elliot AJ, Chalmers RM, Douglas A, Gharbia S, et al. Impact of the COVID-19 pandemic on gastrointestinal infection trends in England, February-July 2020. BMJ Open. 2022; 12: e050469.
- Schmitz J. Is celiac disease a lifelong disorder? Clin Invest Med. 1996; 19: 352-356.
- Hall NJ, Rubin G, Charnock A. Systematic review: adherence to a gluten-free diet in adult patients with coeliac disease. Aliment Pharmacol Ther. 2009; 30: 315-330.
- Matysiak-Budnik T, Malamut G, de Serre NPM, Grosdidier E, Seguier S, et al. Long-term follow-up of 61 coeliac patients diagnosed in childhood: evolution toward latency is possible on a normal diet. Gut. 2007; 56: 1379-1386.
- Hopman EGD, von Blomberg BME, Batstra MR, Morreau H, Dekker FW, et al. Gluten tolerance in adult patients with celiac disease 20 years after diagnosis? Eur J Gastroenterol Hepatol. 2008; 20: 423-429
- Norsa L, Branchi Federica, Bravo M, Ferretti F, Roncoroni L, et al. Celiac Disease 30 Years after Diagnosis: struggling with Glutenfree Adherence or gaining Gluten Tolerance? Journal of Pediatric Gastroenterology and Nutrition. 2018; 67: 361-366.
- Mäki M, Lähdeaho ML, Hällström O, Viander M, Visakorpi JK. Postpubertal gluten challenge in coeliac disease. Arch Dis Child. 1989; 64: 1604-1607.
- Burgin-Wolff A, Gaze H, Hadziselimovic F, Huber H, Lentze MJ, Nusslé D, et al. Anti-gliadin and anti-endomysium antibody determination for coeliac disease. Arch Dis Child. 1991; 66: 941-947
- Anderson RP, van Heel DA, Tye-Din JA, Barnardo M, Salio M, et al. T cells in peripheral blood after gluten challenge in coeliac disease. Gut. 2005; 54: 1217-1223.
- Lähdeaho M-L, Maki M, Laurila K, Huhtala H, Kaukinen K, et al. Small-bowel mucosal changes and antibody responses after low- and moderate-dose gluten challenge in celiac disease. BMC Gastroenterology. 2011; 11: 129.
- Leffler D, Schuppan D, Pallav K, Najarian R, Goldsmith JD, et al. Kinetics of the histological, serological and symptomatic responses to gluten challenge in adults with coeliac disease. Gut. 2013; 62: 996-1004.
- Sarna VK, Skodje GI, Reims HM, Risnes LF, Dahal-Koirala S, et al. HLA-DQ : gluten tetramer test in blood gives better detection of coeliac patients than biopsy after 14-day gluten challenge. Gut. 2018; 67: 1606-1613.
- Goel G, Daveson AJM, Hooi CE, Tye-Din JA, Wang S, et al. Serum cytokines elevated during gluten-mediated cytokine release in coeliac disease. Clin Exp Immunol. 2020; 199: 68-78.
- Schuppan D, Mäki M, Lundin KEA, Isola J, Friesing-Sosnik T, et al. A Randomized Trial of a Transglutaminase 2 Inhibitor for Celiac Disease. N Engl J Med. 2021; 385: 35-45.
- Leonard MM, Silvester JA, Leffler D, Fasano A, Kelly CP, et al. Evaluating Responses to Gluten Challenge: A Randomized, Double-Blind, 2-Dose Gluten Challenge Trial. Gastroenterology. 2021; 160: 720-733.e8
- McMillan SA, Watson RP, McCrum EE, Evans AE. Factors associated with serum antibodies to reticulin, endomysium, and gliadin in an adult population. Gut. 1996; 39: 43-47.
- Choung RS, Khaleghi S, Cartee AK, Marietta EV, Larson JJ, et al. Community-Based Study of Celiac Disease Autoimmunity Progression in Adults. Gastroenterology. 2020; 158: 151-159.e3
- Simell S, Hoppu S, Hekkala A. Fate of five celiac disease-associated antibodies during normal diet in genetically at-risk children observed from birth in a natural history study. Am J Gastroenterol. 2007; 102: 2026-2035.
- Liu E, Dong F, Barón AE, Taki I, Norris JM, et al. High Incidence of Celiac Disease in a Long-term Study of Adolescents With Susceptibility Genotypes. Gastroenterology. 2017; 152: 1329- 1336.
- Auricchio R, Mandile R, Del Vecchio MR, Scapaticci S, Galatola M, et al. Progression of Celiac Disease in Children With Antibodies Against Tissue Transglutaminase and Normal Duodenal Architecture. Gastroenterology. 2019; 157: 413-420.
- Latorre M, Green PHR. The Role of Corticosteroids in Celiac Disease. Digestive Diseases and Sciences 2012; 57: 3039-3041.
- Goel G, King T, Daveson AJ, Andrews JM, Krishnarajah J, et al. Epitope-specific immunotherapy targeting CD4-positive T cells in coeliac disease: two randomised, double-blind, placebo-controlled phase 1 studies. Lancet Gastroenterol Hepatol. 2017; 2: 479-493.
- Vasudevan A, Lubel JS. New-onset of celiac disease during interferon-based therapy for hepatitis. C. Gastroenterol Rep (Oxf). 2015; 3: 83-85.
- Badran YR, Shih A, Leet D, Mooradian MJ, Coromilas A, et al. Immune checkpoint inhibitor-associated celiac disease. Journal for Immunotherapy of Cancer. 2020; 8: e000958.
- Valitutti F, Cucchiara S, Fasano A. Celiac disease and the microbiome. Nutrients. 2019; 11: 2403.
- Hall NJ, Rubin A, Charnock A. Systematic review: adherence to a gluten-free diet in adult patients with coeliac disease. Alimentary Pharmacology & Therapeutics. 2009; 30: 315-330.